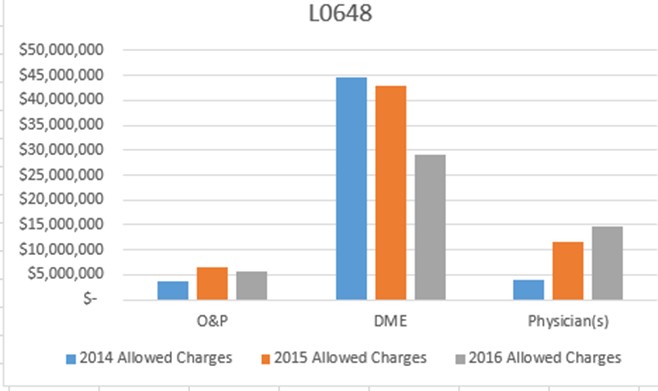
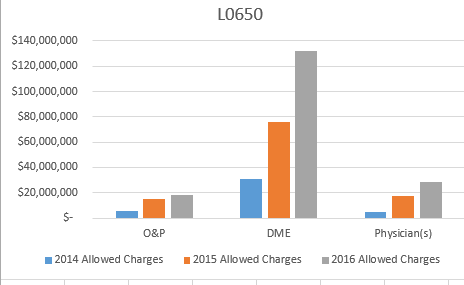
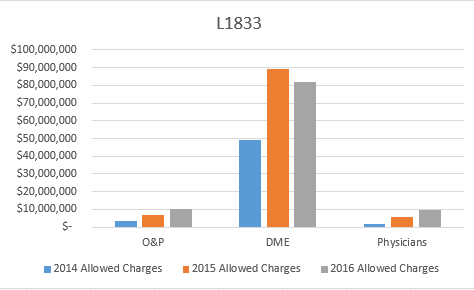
CMS and VA Announce Partnership to Strengthen Prevention of Waste, Fraud, and Abuse Efforts
On January 23, 2018, the Centers for Medicare and Medicaid Services (CMS) and the US Department of Veterans Affairs (VA) announced a new partnership in which they will share data, data analytics and best practices in an effort to improve both agencies efforts to combat waste, fraud, and abuse in their respective healthcare delivery systems.
The VA and CMS represent the two largest public-private healthcare organizations in the country. According to the press release, the partnership will allow the VA to take advantage of gains in data analytics developed by CMS through its Center for Program Integrity.
While the press release discussed general efforts to improve efforts to eliminate waste, fraud, and abuse and made no specific mention of orthotics and prosthetics, the announcement is a clear indication that the VA will be placing increased scrutiny on all providers in the future. While AOPA supports efforts to eliminate fraud and abuse within the healthcare sector, it must be done in a manner that does not inadvertently lead to unnecessary restriction to access to medically necessary care for veterans and Medicare beneficiaries.
View the CMS/VA press release.
Questions regarding this issue may be directed to Joe McTernan at jmcternan@aopanet.org or Devon Bernard at dbernard@aopanet.org.